E406
Joint, Tendon, Ligament, Bone, and Foot Problems
foot | pastern
and fetlock | canon bone regions
| knee and upper front limb | hock
| stifle and upper hind limb | neck
region | different joints and
locations | nutrition and supplements
Introduction:
Today’s horse is a
highly trained athlete that is often pushed to the very limits. Because of this,
tendon, bone, hoof, and joint problems are some of the most common injuries many
horse owners encounter. One of the keys to identifying and then treating these
problems is understanding the terms and anatomical structures that may be
involved. Another key is understanding the function of certain tendons,
ligaments, and bones. To help understand these structures and their function,
the pictures and captions on pages A28, A30, and
A35 are essential. The
following diagrams and definitions are also of benefit.
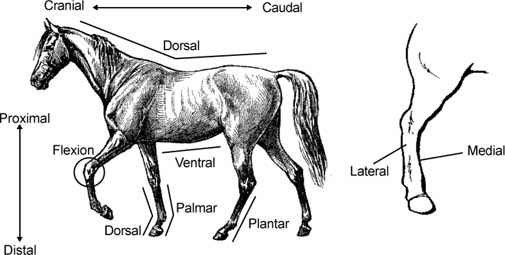
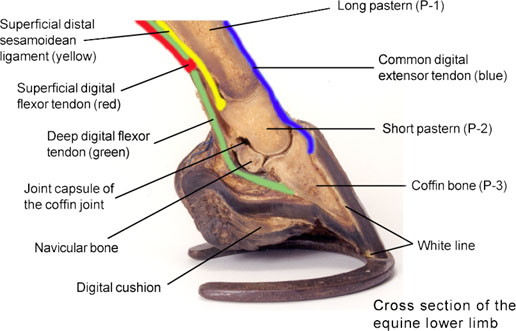
Terms:
- Cranial - Describing something that is closer to the head. For
example, the withers are cranial to the tail.
- Caudal - Describing something that is closer to the tail. For
example, the withers are caudal to the neck.
- Dorsal - Something that is away from the ground or the front
surface of the limb below the knee or hock. For example, the withers are dorsal to the
heart.
- Ventral - Something that is towards the ground. For example, the
udder of a mare is found on the ventral portion of the abdomen.
- Palmar - Describing the back surface of the front limb below the
knee. It is opposite the dorsal surface.
- Plantar - Describing the back surface of the hind limb below the
hock. It is opposite the dorsal surface.
- Proximal - Describing something that is closer to the main part of
the body. For example, the knee (carpus) is proximal to the fetlock.
- Distal - Describing something that is further away from the main
part of the body. For example, the fetlock is distal to the knee (carpus).
- Medial - Something that is towards the middle of the body or limb.
The medial surface of the limb is towards the inside.
- Lateral - Something that is away from the body or limb. The
lateral surface of the limb is towards the outside.
- Deep - Describing something that is farther from the surface. For
example, the cannon bone is deep to the skin surface.
- Superficial - Describing something that is closer to the surface.
For example, the skin is superficial to the gluteal muscles.
- Tendon - A tendon is a fibrous cord that attaches muscle to bone.
Tendons are used to flex and extend each joint when a muscle or group of muscles
contracts. Some of the most common tendons that can be injured in the horse are
the flexor tendons (superficial and deep flexor tendons) in the distal and
palmar/plantar areas of the front and hind limbs.
- Ligament - This is a band of fibrous tissue that connects bone and
cartilage. It is often referred to as the connection from bone to bone.
- Joint - The place where two or more bones of the body join.
- Cartilage - A specialized connective tissue that is found on the
ends of bones that form part of a joint.
- Synovial Membrane - The inner lining of the joint capsule or
tendon sheath that contains the synovial or joint fluid.
- Synovitis - Inflammation of the synovial membrane.
- Arthroscope/arthroscopic Exam - An arthroscopic exam is a
procedure where a specialized instrument called a arthroscope is inserted into a
joint. The arthroscope is a long slender instrument with a fiber optic camera on
the end of it that transmits a picture to a viewing screen.
- Arthritis - This means inflammation of a joint. The inflammation
can be caused by injury, degeneration, or infection.
- Physis/physitis - The growth plate of a bone. When it becomes
inflamed, it is called physitis.
- Epiphysitis - In specific terms, this relates to inflammation of
the end of a long bone. There is a disease called epiphysitis that is actually a
problem with the growth plate.
- Bone - The hard form of connective tissue that makes up most of
the skeleton.
- Degenerative Joint Disease (Osteoarthritis) - Degenerative joint
disease (DJD) is the final outcome of many different problems that occur in the
joint. A joint with DJD has destructive changes in the cartilage, bone, and
tissues. These changes can be caused by arthritis, synovitis, injury,
osteochondritis, fractures, etc.
- Osteochondritis - Inflammation of both bone and cartilage.
- Periosteum - Specialized connective tissue that covers the bones
in the body. It is essential for proper bone growth and continued bone support.
- Ankylosis - When a joint is made immovable by disease, injury, or
surgical procedure.
- Arthrodesis - When a joint is surgically fused/joined to prevent
movement.
Diagnosing a Problem:
Many times it is
obvious that an injury has occurred. Other times the injury may be old, or the
horse may not be showing significant signs of lameness. The suggestions,
pictures, and information found on pages B885 and
E460 can help a horse owner
identify a lameness problem.
The following information will identify the specific tendon, ligament, joint,
bone, and foot problems that are common in horses. For the most part, the
information will be broken down into sections based on anatomical location of
where the problem is occurring. For example, all problems associated with
fetlock will be discussed together in alphabetical order. A general category is
found towards the end that contains problems that can be found in many different
joints or locations. Details on the cause, clinical signs, diagnosis, and
treatment of each problem will be included as needed. A brief discussion on the
role of nutrition and supplements in bone and joint problems is also found at
the end of the discussion.
Note: The following reference has been used extensively to generate much of
the information contained in this discussion: Ted S. Stashak, DVM, MS. Adams’
Lameness in Horses. Lea and Febiger, 1987.
Problems with the Foot
- Abscesses, Bruising, and Puncture Wounds:
Causative Agents: Foot abscesses are pockets of infection that occur
under the sole or hoof. They can be caused by bruising from rocks or hard
objects that impact the sole of the foot. If the bruising is severe, the
sensitive tissues can die (necrose) and an abscess will result. Abscesses can
also occur with laminitis and puncture wounds.
Clinical Signs: These horses are often lame on the affected limb and
are sensitive to hoof testers in the injured area. Areas of heat may also be
noted in the foot. If the abscess is open, it will have some discharge (either
serum or infection). In many cases the outer surface of a bruise or abscess can
be removed with a hoof knife, revealing red staining (hemorrhage) in the
underlying tissues. If the problem is caused by a puncture wound, a tract or
maybe even the nail or other object can be seen. If the nail is still in place,
it is best not remove it until a veterinarian can examine the extent of the
puncture with a radiograph (X-ray). If the abscess or infected puncture wound
does not have a place to drain, it may "break out" at the coronary
band. This appears as an open wound, draining infectious material.
Treatment: The outer surface of an abscess must be removed to allow
draining and any bruised tissue should be removed. Puncture wounds should also
be explored and any associated abscess drained. If the puncture wound involves
any bone or joint structures, extensive treatment involving flushing, surgical
draining, and antibiotics are required. Sometimes portions of the hoof wall need
to be removed to allow adequate draining. (This requires training and sometimes
special equipment.) Once the abscess/puncture wound is opened and clean, the
foot should be soaked on a daily basis in a solution of dilute betadine or epsom
salts for 10-15 minutes. After soaking, antiseptic (betadine) ointment should be
applied to the draining wound, a gauze pad placed over the area, and the foot
wrapped to prevent additional contamination. Covering the bottom of the foot
with duct tape can help reduce the contamination and keep the bandage in place.
Keeping the foot clean and dry is a must until the injury has healed. Giving the
horse a tetanus shot, particularly if a puncture wound is involved, is
important. It is best to rest these animals from any strenuous work until
adequate healing takes place.
Corns:
Causative Agents: Corns are caused by pressure placed on the wall and
sole of the foot in the heel regions. This pressure can come from improper
shoeing or by letting the feet get too long with the shoe in place.
Clinical Signs: These horses are often lame on the affected limb and
are sensitive to hoof testers in the heel area. The corn can be dry or have some
discharge (either serum or infection). In many cases the outer surface of the
corn can be removed with a hoof knife, revealing red staining (hemorrhage) in
the underlying tissues.
Treatment: If the problem has been caused by improper shoeing,
removing the shoe is a must. If the corn has some discharge, the outer surface
of the corn must be removed to allow draining and any bruised tissue should be
removed. Once the corn is drained, the foot should be soaked on a daily basis in
a solution of epsom salts for 10-15 minutes. After soaking, betadine ointment
should be applied to the corn area and the foot wrapped to prevent additional
contamination. Covering the bottom of the foot with duct tape can help reduce
the contamination. Keeping the foot clean and dry is a must until the injury has
healed. If the horse must be used, a bar type shoe should be put on the foot.
These types of shoes help to distribute the horse’s weight evenly around the
foot and to the frog, reducing the amount of pressure placed on the heel
regions. If necessary, the corn should be trimmed away to avoid contact and
pressure with the shoe.
Dry Hoof Wall:
Introduction and Recommendations: The amount of moisture in the hoof
wall is influenced by the environment and the amount of moisture in the ground.
When the environment is dry, with little moisture, the feet can become brittle.
Nutrition can play a role in maintaining healthy feet; if the horse is fed a
balanced diet with appropriate amounts of protein and energy, the feet will not
usually suffer.
General ingredients that keep the foot moist are pine tar, lanolin, fish
oils, and olive oil. Select products in which these are the active ingredients.
Pine tar products seem to be the most effective and generally cost the least.
Other ingredients like ketones, toluene, acetate, and alcohols are commonly
used, but are not as effective.
Fractures:
Causative Agent: Fractures of the coffin bone or P-3 are not very
common. When they do occur, they are often the result of strenuous exercise on
firm or packed ground. A fracture of the extensor process of the coffin bone can
also occur. Extensor process fractures occur when excessive stress is placed on
the common digital extensor tendon or when the coffin joint is placed in severe
extension.
Clinical Signs/Diagnosis: Severe lameness is often noted with
fractures of the coffin bone. This is not so obvious with fractures of the
extensor process. If a fractured extensor process has been a problem for some
time, the foot may actually take on a sort of V-shape. Radiographs are the best
way to diagnose each of these problems.
Treatment: Most fractures of the coffin bone can be treated by placing
on a full bar shoe with quarter clips on both sides. This will help prevent the
expansion of the hoof wall. Strict stall rest for 8-10 months is essential for
complete recovery. The best treatment for a fractured extensor process is
surgical removal or possibly screwing a large fragment back onto the coffin
bone. No matter what procedure is used, strict stall rest is essential for 8
weeks. After this time, the horse should be rested and only hand walked for an
additional 6 months.
Laminitis (Founder) - For a discussion on laminitis, refer to page E465.
Navicular - For a complete discussion on navicular, refer to page E544.
Pedal Osteitis:
Causative Agent and Diagnosis: Repeated and chronic inflammation of
the coffin bone causes this problem. This continued inflammation can be caused
by laminitis, sole bruising, puncture wounds, and corns. The continued
inflammation causes the outside edges of the coffin bone to demineralize. These
areas of demineralization can be seen on radiographs as places where the edges
of the coffin bone look roughened and "moth eaten."
Clinical Signs and Diagnosis: Lameness is often noted with this
problem of the coffin bone, and the horse can be sensitive to hoof testers in the
toe region.
Treatment: Most cases of pedal osteitis can be helped by using shoes
and padding that keep the sole from impacting the ground. Treating the
underlying problem (laminitis, bruising, etc.) causing the inflammation is also
essential. Rest is necessary for a complete recovery; however, some animals may
never return to full function.
Quittor:
Causative Agent: This problem is caused when an injury takes place
near the coronary band over the areas of the collateral cartilages. The
collateral cartilages are found on either side of the coffin bone of the foot
and extend up past the coronary band. These injuries introduce infection into
the cartilages.
Clinical Signs: Swelling, pain, and heat are often noted over the
coronary band. Draining tracts of infection can often be found above the
coronary band. These horses can be lame early on, but show fewer signs as the
problem progresses.
Diagnosis: Many other problems can also cause draining at the coronary
band (gravel, abscesses). The difference between quittor and these other
problems is the fact that this problem is more extensive and the draining tracts
are often larger and extend deep in the foot. The draining tracts will often
come and go. Radiographs can also be helpful in identifying this problem.
Treatment: Surgical removal of the problem cartilage is the best
treatment. All the draining tracts are also removed. Flushing, soaking, and
antibiotics are continued treatments after the surgery.
Selenium Toxicity - This can cause the hoof wall to crack parallel to
the coronary band in different sections down the hoof wall. Other problems can
also be noted in the coat, mane, and tail. Additional details on selenium
toxicity can be found on E835.
Sheared Heels:
Causative Agents: This condition occurs when there are abnormal forces
applied to one of the heel bulbs. This over use of one of the heels occurs when
improper trimming causes one heel to be left longer than the other. Because one
heel is used more often than the other, a breakdown of the tissues and
structures between the heel bulbs occurs. Horses with long toes and short heels
are also susceptible.
Clinical Signs/Diagnosis: Most horses with sheared heels can be
identified by examining the back portion of the foot. The heel that is left too
long is thrust upwards and has a straighter hoof wall when compared to the
opposite heel (see figure 1). The heel that is not bearing the excessive weight
often has a flared hoof wall. Pain is sometimes noted when the heel bulbs are
pushed in opposite directions. Hoof testers can also be used to identify areas
of pain in the heel regions.
Figure 1

|
|
|
| The
heel on this side is the one bearing most of the weight. It has a straight wall
and the coronary band above this heel is thrust upward. |
|
Treatment: The key to treating this problem is to bring the foot back
into balance by trimming the long heel. Some cases may resolve by simply
trimming and then letting the horse go bare foot. In other cases, the long heel
should be trimmed and a full bar shoe should be used to distribute the horse’s
weight evenly around the foot. With successive trimming and shoeing, the foot
can eventually come back into balance with both heels evenly on the ground
surface. In very severe cases, a normal return to function may not be
achieved.
Sidebone:
Causative Agent: Sidebone is caused by concussion forces being placed
on the collateral cartilages. The collateral cartilages are found on either side
of the coffin bone of the foot and extend up past the coronary band. With
continued traumatic forces, the collateral cartilages begin to turn to bone (or
ossify). Sidebone is usually found in the front feet of horses that have
conformation problems. Animals that are base-narrow or base-wide have the
tendency to develop this problem.
Clinical Signs: Pain and heat are often noted over the collateral
cartilages during the active stages of the disease. The cartilages that are
involved will often be harder than normal and painful to the touch. These horses
may or may not be lame.
Diagnosis: It is often easy to falsely conclude that sidebone is the
cause for a horse’s lameness. Sidebone should not be diagnosed as the cause of
lameness unless there is heat and pain associated with the collateral
cartilages. Radiographs showing the cartilage turning into bone can be used to
identify this problem. This finding alone, however, is not sufficient to
diagnose sidebone without the associated signs of heat and pain.
Treatment: Some farriers recommend that the hoof wall over the
sidebone areas be thinned or grooved. These processes allow the foot to expand
and be more flexible. If fractures of the sidebone occur, they need to be
surgically removed. If pain and heat are still present, treating with
phenylbutazone can help. All cases should be rested until the inflammation has
subsided. In general, many cases are not lame and do not require treatment
unless there is active pain and heat.
Thrush:
Causative Agent: Thrush is caused by an infection of anaerobic bacteria and
potentially other organisms in the frog and sulcus (commissure). These organisms
infect horses that are kept
in moist, dirty environments, where the foot is continually dirty and wet. Feet
that are improperly shod or are improperly trimmed are also at risk of being
infected.
Clinical Signs: In most cases the commissures of the foot are full of a
dark, foul smelling discharge. The commissures are often deeper than normal, and
the frog can be loosened from the underlying tissues. In severe cases the
organisms can be infecting the sensitive structures of the foot causing lameness
and infections going up the limb.
Treatment: The treatment for thrush involves keeping the foot clean, dry,
and properly shod. After the foot is completely cleaned with a hoof pick and
knife, topical medications such as povidone-iodine (Betadine), chlorhexidine, or
Kopertox should be applied on a daily basis until the infection is cleared.
Toe, Quarter, and Heel Cracks (Sand cracks):
Causative Agent: Cracks can start from the bottom or the top of the hoof
wall and extend variable distances. The cracks that start at the coronary band
are usually caused by some type of trauma or injury to the coronary band. The
cracks that start at the bottom of the foot are most often caused by letting the
foot go too long without trimming. Excessive drying of the foot can also make it
more susceptible to cracking.
Clinical Signs: Depending on the severity of the cracks, some horses may
be lame. Some cracks may become infected and discharge blood or pus.
Treatment: The treatment for each crack will depend on its location,
depth, and how far up or down the hoof wall it extends. Any cracks with signs of
infection, should be treated with povidone-iodine (Betadine) and bandaged until
the infection is cleared. Current treatments for many cracks involves the use of
synthetic epoxy and hoof repair materials. Before these materials are placed in
the crack, the crack should be thoroughly cleaned and possibly burred out to
enlarge the area for the glue or plastic to adhere. Some horses should be shod
with toe clips placed on either side of the crack to prevent it from expanding (see figure
2).
Figure 2

|
White Line Disease (Gravel):
Causative Agent: This problem is caused when an opening or defect in
the white line occurs. This can result from an excessively dry foot or when a
puncture wound, rock, or piece of gravel damages the white line. The opening in
the white line allows infection (not the piece of gravel) to migrate up the hoof
wall through the sensitive structures and drain at the coronary band.
Clinical Signs: White line disease is usually first identified when a
draining tract of infection is noticed at the coronary band; however, some
horses can be lame before the draining at the coronary band ever takes place. If the underside of the foot is examined, a spot or area of blacked
tissue can often be seen in the white line. These areas indicate where the
defect in the white line occurred.
Diagnosis: As mentioned earlier, other problems can also cause draining
at the coronary band (quittor, abscesses). The difference between white line
disease and these others is that it involves the white line from the sole to the coronary band.
Probing and examination of the black spots found in the white line often help
identify white line disease as the problem.
Treatment: The treatment for white line disease is essentially the
same as the treatment for abscesses and puncture wounds.
Problems in the Pastern and Fetlock
- Fractures of the Middle Phalanx (P-2):
Introduction and Causative Agents: Fractures of P-2 can be anything from
a chip fracture to a comminuted (multiple pieces) fracture. When they do occur,
they are often the result of strenuous exercise on firm or packed ground. This
usually happens with middle-aged horses that are used for barrel racing,
cutting, roping, and reining. The hind limbs are more often affected than the
front limbs.
Clinical Signs and Diagnosis: Severe lameness is often noted with these
fractures. Occasionally a "pop" is heard just prior to the horse
becoming extremely lame. In most cases, swelling, pain, and crepitus
("grinding") can be noted just above the coronary band when the area is
handled and the pastern manipulated. Radiographs are the best way to diagnose
each of these problems.
Treatment: Chip fractures can be treated with surgical removal or by
just treating the clinical signs in some minor cases. If one large piece of P-2
is fractured, or if the fracture is comminuted (has multiple pieces), it may be
treated with screws, casting, or by arthrodesis of the joint. All animals are
placed on strict rest for multiple weeks. Many of the more serious fracture
victims do not return to riding condition for 9-12 months. If the fracture is
comminuted, a poor return to normal function should be expected.
Fractures of the Proximal Phalanx (P-1):
Introduction and Causative Agents: Fractures of P-1 are most commonly
a fissure type fracture (a crack that does not go completely through the bone)
or a comminuted (multiple pieces) fracture. These fractures occur when twisting
forces are placed on the limb while bearing weight. This can happen when the
horse makes a sharp turn.
Clinical Signs and Diagnosis: Severe lameness is often noted with
comminuted fractures, while the fissure type fractures have various levels of
lameness. In most cases, swelling, pain, and crepitus ("grinding") can
be noted when the area is handled and the fetlock manipulated. Radiographs are
the best way to diagnose the extent and type of damage.
Treatment: The ideal way to treat many of these fractures is by using
bone screws to put the fractured pieces back together (internal fixation). This
surgery is then followed by casting and strict stall rest for many weeks. Many
of the more serious fracture victims do not return to riding condition for 9-12
months, and if the fracture is comminuted, a poor return to normal function
should be expected.
Ringbone:
Introduction and Causative Agent: Ringbone is the abnormal growth of new
bone that forms on the long pastern, short pastern, or coffin bone (proximal,
middle, or distal phalanx). When this bone growth occurs on the long pastern and
the top (proximal) end of the short pastern, it is called high ringbone. When it
occurs on the lower (distal) end of the short pastern and the coffin bone, it is
called low ringbone. Ringbone can be found in horses that make quick stops and
twisting turns at high speeds (performance, polo, etc.). It is also common in
draft type horses that are not worked at speeds, but have a "boxy"
conformation in the pastern.
Ongoing inflammation of the periosteum (periostitis) that covers each bone
causes high and low ringbone. When the periosteum is inflamed, the horse’s
body lays down new bone in the inflamed area. The inflammation of the periosteum
can be caused by pulling and stress on the joint capsule, tendons, and ligaments
that are found in these areas. A fracture to any of the bones in this region can
cause ringbone to form. A wound that involves the periosteum can also cause
ringbone. Often, it is the poor conformation of the horse that causes the excess
stress on the joint capsule, tendon, or ligament.
Clinical Signs and Diagnosis: These horses are often lame and may have
swelling, heat, and pain associated with the locations of the ringbone. These
areas may be firm and irregular to the touch. Ringbone problems most often occur
in the front limbs. If low ringbone affecting the extensor process of the coffin
bone is the problem, the foot may take on "buttress foot" appearance.
A buttress foot is one where the excess bone causes the top (dorsal) surface of
the foot around and above the coronary band to bulge. The shape of the hoof wall
can also be distorted. To diagnose ringbone, a radiograph must be taken. On the
radiograph, evidence of excess bone production and arthritis can be noted.
Treatment: The treatment for ringbone is based on preventing any
additional movement to the joint(s) in the involved areas. This sometimes occurs
naturally when the bones on either side of a joint fuse and cause ankylosis of
the joint. There are different surgical procedures that can accomplish the same
fusing or athrodesis of the joint. Some horses never return to full function
even with surgery, and attempts to manage this disease without surgery are
usually unsuccessful. The key to successful treatment involves diagnosing this
problem early and implementing appropriate treatment in a timely manner.
Windpuffs and Thorough-pin:
Introduction and Causative Agents: Windpuffs is the common term for
inflammation of the synovial membrane lining the fetlock and the digital flexor
tendon sheath. Tenosynovitis is the term used to describe inflammation of the
synovial membrane (synovitis) lining of the tendon sheath. Windpuffs can sometimes be a
combination of synovitis and tenosynovitis. When these structures become
inflamed, excess joint fluid is produced and the joint capsule/tendon sheath
expands. Injury to the fetlock joint causes the inflammation. These injuries are
often the result of poor conformation (straight fetlocks) or heavy training.
Clinical Signs: The excess fluid causes a soft, fluid-filled bulge to
appear just above the fetlock joint, behind the back of the cannon bone (see
figure 3). This swelling is not hot, and the horse should not be in pain or
lame.
| Figure 3: Mild windpuffs |
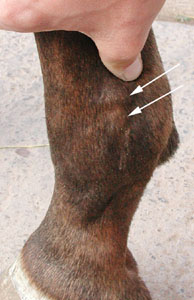 |
Treatment: In many cases, resting the horse will help alleviate the
problem. In younger horses, the problem will often leave as the horse grows.
Pressure wraps and topical DMSO can be used if the problems persist.
Thorough-pin is the common term for tenosynovitis in the tarsal sheath that
surrounds the deep digital flexor tendon in the hind limb. This condition can be
identified by noting swelling of the tendon sheath above the fetlock on the back
of the hind limb. Thorough-pin is a mild form of tenosynovitis and should be
treated like a horse with windpuffs. Like windpuffs, the swelling in
thorough-pin is not hot, and the horse should not be painful or lame. Often the
cause of thorough-pin is not known.
Problems in the Cannon Bone Regions (Metacarpus, Metatarsus, and Splint
Bones)
- Fractures:
Introduction and Causative Agents: Fractures of cannon bone and splint
bones can be anything from a fissure fracture to a comminuted (multiple pieces)
fracture. These fractures are most commonly caused by traumatic injury due to
kicks, falls, slipping, and other accidents. In foals this injury can be caused
by the mare stepping on the foal. Splint fractures are usually the result of
interfering or a kick from another animal.
Clinical Signs and Diagnosis: Non-weight bearing lameness is often noted
with fractures of the cannon bone. In most cases, swelling and pain can be found
in the cannon area. Radiographs are the best way to diagnose each of these
problems. See the discussion on "splints" for more details on clinical
signs and diagnosing this problem.
Treatment and Prognosis: For treating many of the uncomplicated fractures
or fissures, a cast is often used. If one large piece is fractured, or if the
fracture is comminuted (has multiple pieces), it may be treated with screws,
pins, and plates. Many times a cast is applied after the surgery to help provide
support to the healing bone. Fractures of the splint bones are usually removed
surgically. All animals are placed on strict rest for multiple weeks. Many of
the younger horses with these types of fractures do fairly well after successful
treatment. If the horse is older, the fracture has broken the skin, or the
fracture is comminuted, the prognosis is poor.
Splints:
Causative Agents and Clinical Signs: "Splints" are basically
fibrous and/or boney proliferation that takes place between the splint bones and
the cannon bone. Each splint bone is attached to the cannon bone by an
interosseous ligament. Anything that causes stretching or tearing of the
ligament and inflammation in these areas can cause splints to occur. A fracture
of the splint bone can also result in a lesion. When inflammation is present,
periostitis of the splint bone occurs and a splint will develop. Splints
appear as firm to hard lesions near or on the splint bone itself (see figure 4).
In the early stages, the horse may be lame and the splint may be painful and
swollen. As the initial inflammation subsides, the lesion may actually decrease
in size, but become more firm. This problem most often occurs in the front
limbs. Most splints are caused by four major things: interfering (trauma), over
nutrition (calcium and phosphorus imbalances), over-working, or poor
conformation (bench knees, or really base narrow and/or toed-out horses).
| Figure 4: Splint |
 |
Diagnosis: Many cases can be identified by the clinical signs (location,
swelling, heat, and pain). If a fracture of the splint is involved, the swelling
and pain may be more extensive and severe. In some cases radiographs will need
to be taken to determine if a joint or the cannon bone is involved. If
interfering is suspected, place white chalk on the inside hoof of the opposite
limb. Work the horse and watch for evidence of chalk on the splint area.
Treatment: The treatment will vary depending on the cause; therefore, it
is important to determine the exact cause of the splints. For interfering
problems, using good splint boots will help resolve the problem. The idea behind
splint boots is to prevent the opposite limb from contacting the shin (cannon)
area. These boots contain some type of thickened material for protection. The
key to placing the boots is not necessarily how tight they are, but that they are placed properly to protect the shin
(cannon) bone areas. The horse should also be evaluated (by owner and farrier)
for any trimming or shoeing reasons for the horse to interfere. Most
conformation problems are difficult to correct. If nutrition in a young horse
might be the problem, use the information on page A575 to calculate what is
being fed. If the ration seems too hot, take measures to decrease the amount of
energy (TDN) being fed.
Anti-inflammatory agents (bute,
topical DMSO) and cold water soaks are essential for splints that are painful, tender, and
swollen. Cold water/ice can be applied
20 minutes twice a day for 5-7 days. After the soaks, pressure wrapping the
involved areas can also help. Rest is also essential until the inflammation has
gone down (30-45 days). If the splints are more chronic (have been going on for
some time), the above may not be useful. In these cases the extra bone may have
to be removed by surgery. In general, if the initial inflammation is reduced
early on, the outcome is usually favorable. It is also essential to remove the
cause (nutrition problems, interfering, etc.). Most splints resolve with time
and proper treatment.
Stress Fractures, Bucked Shins, and Shin Splints of the Cannon Bone:
Introduction and Causative Agent: All of these terms are used
to describe injury to the cannon bone that takes place when severe compression
forces are placed on the limb during impact. When bone remodeling cannot keep
up with the repeated stresses, defects in the bone occur. These injuries most
often occur in young animals (2-3 years of age) that are under extensive
training programs.
Clinical Signs and Diagnosis: In the acute, mild form of the disease,
the horse may be in pain when pressure is placed on the involved area of the
cannon bone. The horse is usually only sightly lame and the condition may even
go unnoticed. If the problem progresses, swelling may be felt on the
front/middle (dorsomedial) surface of the cannon bone. The pain is usually more
severe at this stage. In the early part of this problem, radiographs are often
normal. As the problem progresses, radiographs may show a subperiosteal callus
forming in the injured areas of the cannon bone. These calluses are the way the
bone tries to heal itself by laying down extra bone for added strength.
Occasionally, fractures are observed on a radiograph.
Treatment: For the more mild cases, rest and daily hand walking are
recommended. This should be continued until the cannon bone is no longer painful
to pressure. After this, the horse can be placed on a controlled exercise
program. The length and duration of the controlled exercise program is
determined by how well the cannon remains unpainful. Anti-inflammatory agents
are also of benefit. For the more severe cases, the extent of rest may go as
long as one year. There are some surgical procedures for those cases that do not
respond to rest and anti-inflammatory agents.
Problems in the Knee (Carpus) and Upper Front Limb:
- Fractures:
Introduction and Causative Agents: Most of the fractures in the knee are
associated with the small carpal bones and end of the radius that form the
joint.
Horses that jump, race, and do athletic performances are prone to developing
these types of fractures. When horses perform these types of activities, the
knee is under significant amounts of compressive pressure. These forces result
in chip, slab, and comminuted fractures. Direct injury from a kick or blow can
also cause a fracture.
Clinical Signs and Diagnosis: Swelling, pain, and lameness are common
signs. Physical examination using flexion tests and injections of anesthetic
into the joint can help identify a knee problem. To determine the exact location
of the fracture, radiographs are essential.
Treatment and Prognosis: Small chip fractures that are still adhered to
the larger piece of bone can often be treated with rest and anti-inflammatory
agents. The horse should be confined for 6-12 weeks and then hand-walked for
another 6 weeks. Large chip fractures can be treated with surgical removal.
After surgery, they should be rested for 6-7 months. A slab fracture can be
treated with a screw or surgically removed. These animals should also be rested
for 6-7 months. Surgical treatment for comminuted fractures is often
unsuccessful and is only used for animals that have breeding potential. Many
chip fractures that are treated early and properly, have a good return to normal
function. However, most of the slab and particularly the comminuted fractures
have a poor prognosis.
Fractures in the Upper Front Limbs:
Introduction and Causative Agent: Fractures of the radius, ulna,
humerus, and scapula will be discussed below. Other fractures in the lower limbs
have already been discussed and fractures in the hind limbs will be discussed
latter. In general, fractures that occur in foals have a greater chance of being
treatable. Direct injury or trauma to the area is usually the cause of these
fractures. This injury can come from a kick or accident (collision). The
resulting injury can be anything from a fissure fracture to a comminuted
(multiple pieces) fracture.
Clinical Signs and Diagnosis: Non-weight bearing lameness is often
noted with these fractures. In most cases, swelling, pain, and crepitus
("grinding") can be found when the area is handled and manipulated.
Diagnosing these injuries is not usually difficult and radiographs are the best
way to determine the extent and type of fracture.
Treatment and Prognosis: For some minor fractures of the ulna, strict
stall rest may be all that is needed for the fracture to heal. More complicated
fractures of the radius and ulna are best treated with surgery. During the
surgery, plates and screws are used to hold the fracture in place. Fractures of
the humerus may be treated with strict stall rest, slinging the horse, and
bandages. Foals respond better to this treatment than do adults. Foals with
humerus fractures may also be treated with pins and potentially plates and
screws. Radial nerve paralysis is sometimes a problem with fractures of the
humerus.
Fractures of the scapula can sometimes be treated with rest, and if
necessary, surgical removal of any small, boney fragments. Some scapula
fractures in foals may be treated with plates and screws. If the fracture of the
scapula involves the shoulder joint, there is often no effective treatment.
No matter what type of fracture has occurred, attention should be given to
the opposite limb. In many cases, the opposite limb will be forced to bear most
of the weight. This can result in laminitis, angular limb deformities, and other
problems.
Many of the younger horses with these types of fractures do fairly well after
successful treatment. If the horse is older, the fracture has broken the skin,
or is comminuted, the prognosis is poor.
Problems in the Hock (Tarsus):
- Bog Spavin:
Introduction and Causative Agents: Bog spavin is the common term for
synovitis in the hock or tarsal joint. Synovitis is inflammation of the synovial
membrane covering the joint. When it becomes inflamed, excess joint fluid is
produced and the joint capsule expands. Repeated injury to the hock joint causes
the inflammation. These injuries are often the result of poor conformation
(straight, cow, or sickle-hocked) or heavy training. Improper shoeing,
fractures, and osteochondritis dissecans (OCD) can also cause this problem. Some
studies show that nutritional imbalances and deficiencies (low calcium, vitamin
D & A, and phosphorus) may also play a role in the development of this
disease. This most commonly occurs in animals 6 months to 2 years of age.
Clinical Signs: The excess joint fluid causes soft, fluid filled
bulges to appear on the inside and outside areas of the hock (see figure 5).
Like windpuffs, these swellings are not hot, and the horse should not be in pain
or lame unless the bog spavin is due to an injury or OCD lesion. As pressure is
placed on one of the swellings, the fluid will be pushed to other swellings and
make them larger.
| Figure 5: Bog spavin |
 |
Diagnosis: It is important to determine the exact cause for the joint
swelling (OCD, trauma, nutrition, etc.). To do this a radiograph is a must.
Treatment: In many cases, resting the horse will help alleviate the
problem. In younger horses, the problem will often leave as the horse grows. If
the problem is due to OCD, surgical treatment of the lesion is necessary. When
nutritional deficiencies are the cause, supplementation is required. If the
problem is severe or the horse is lame and painful, injections of
corticosteroids and other products may be given in the joint. Some of the
anti-inflammatory and glycosaminoglycan products may also be of benefit. Because
no treatment seems to be 100% effective, bog spavin is sometimes a difficult
problem to completely cure. This is particularly true if the problem is caused
by a conformation defect or trauma.
Bone Spavin or Jack Spavin (Degenerative Joint Disease of the Distal
Tarsal Joints):
Introduction and Causative Agents: Bone spavin is found most often in
horses that are ridden at high speeds, where they are used for jumping, reining,
roping, and cutting. Damage and inflammation occurs in the lower bones and
joints of the hock when compression and rotation stresses are placed on the hock
during these exercises. Like bog spavin, these injuries are often the result of
poor conformation (straight, cow, or sickle hocked). Some studies show that
nutritional imbalances and deficiencies may also play a role in this disease.
Clinical Signs/Diagnosis: These horses
often have a history of being moderately lame after exercise, but improve with
rest. These horses are positive to the spavin or hock flexion test. To perform a
spavin test, the limb should be held in this position, with the cannon bone
parallel to the ground, for 1-2 minutes (see
figure 6). Once the limb is released, watch the horse for signs of lameness as
it is trotted away. Because of the inflammation to the periosteum (periostitis),
extra bone is formed over the front and inside areas of the hock joint. As a
result, a firm, boney bump can often be detected on the inside (medial) portion
of the lower hock (see figure 7). Radiographs are very important in diagnosing
this disease. Multiple views of both hocks are often necessary to help identify
the problem.
|
Video clip of a spavin test being performed. |
|
 |
|
If the video
does not play, you must install an MPEG video
player on your computer (e.g. Windows Media Player).
Click here to
download Windows Media Player.
Or
Install Internet Explorer from our CD Manual. |
| Figure 7: Bone spavin |
 |
Treatment: In many cases of bone spavin, treatment efforts are not very
effective. Many horses remain lame and never return to full function. There are
various surgical techniques that can be used to help treat bone spavin. The most
common is a procedure called a cunean tenectomy. This procedure removes the
portion of the cunean tendon where it moves over this region of the hock.
Corrective shoeing can also help many of these horses. The intent of the
corrective shoeing should be to cause the foot to break-over quicker. This can
be accomplished by using a rocker or rolled toed shoe.
Curb:
Introduction and Causative Agents: Curb is a condition where the back
(plantar) aspect of the fibular tarsal bone is enlarged. This results from an
enlargement of the plantar ligament due to inflammation and thickening. In some
cases periostitis is involved and there is an extra layer of bone in that
region. The plantar ligament is located in the area just below the point of the
hock. Inflammation of the plantar ligament is often the result of poor
conformation (straight, cow, or sickle hocked) or when the horse injures itself
in the hock region by kicking against trailers or walls.
Clinical Signs and Diagnosis: Signs of heat, swelling, pain, and lameness
are common early on in the condition. As things progress, scar tissue and an
obvious bump may be noticed (see figure 8). Radiographs can help determine the
cause and extent of a suspected case of curb.
| Figure 8: Curb |
 |
Treatment: In many cases, resting the horse will help alleviate the
problem. Rest should be accompanied by ice packs, anti-inflammatory agents, and
corticosteroid injections under the skin in the area of the lesion. In cases
that have been going on for sometime, successful treatment may not be
achieved.
Problems in the Stifle and Upper Hind Limb
- Patella Problems:
Introduction: The patella is the horse’s knee cap. It can be
fractured, luxated, or become fixated or "stuck."
Causative Agents: Luxations and fractures are due to trauma caused by
kicks and collisions. Luxations can also be due to congenital abnormalities. The
upward fixation of the patella is caused by genetic traits where the horse has a
"straight hind limb" conformation. Poor muscling and muscle tone can
also be part of the problem. In this situation, the patella becomes fixed or
catches on a ridge (medial trochlear ridge) of the femur. This prevents the limb
from flexing.
Clinical Signs and Diagnosis: When luxations and fractures are the
problem, the stifle will be swollen and painful. The horse may show varying
degrees of lameness. Radiographs are also helpful in diagnosing these problems.
If the horse has a problem with upward fixation of the patella, the limb may
actually be "locked" in a flexed position where the stifle and hock
cannot flex. If the horse is only "catching" the patella on the ridge,
the horse will have a jerky gait when turned in a circle or walked up or down a
hill.
Treatment: For luxations and fractures, surgical procedures can be
used to help treat the problem. For minor fractures, stall rest and splints may
be all that is needed. Treatment for a fixed patella depends on how severe it is
and if the patella is "locked" or just "catches." For
immediate treatment of a locked patella, the limb can be pulled forward, while
pressure is placed on the patella to force it down and medially. The horse can
also be backed down a hill, while the same pressure is placed on the patella to
force it down and medially. Some recommend startling the horse, causing the
patella to release. This should be done with caution because of the potential
for additional injury. In the more severe cases, surgery can be performed to cut
the medial patellar ligament. This allows the patella to release and prevents
any additional locking of the patella on the medial trochlear ridge of the
femur. Once the surgery is performed, the horse should not be used for at least
6 weeks.
Prognosis: For luxations, the prognosis is guarded to poor. For fractures
of the patella, the prognosis can be favorable if proper and thorough treatment
is implemented. The prognosis for upward fixation of the patella is good as long
as the joint has not suffered any permanent damage.
The following video clip shows a pony with a fixated
patella in the left hind limb. The patella remains fixated throughout
the entire video.
Fractures in the Upper Hind Limbs:
Introduction: Fractures of the tibia, femur, and pelvis will be
discussed below. In general, fractures that occur in foals have a greater
chance of being treatable. Direct injury or trauma to the area is usually the
cause of these fractures. This injury can come from a kick, severe compression
forces, or accident (collision). The resulting injury can be anything from a
fissure fracture to a comminuted (multiple pieces) fracture.
Clinical Signs and Diagnosis: Non-weight bearing lameness is often
noted with these fractures. In most cases, swelling, pain, and crepitus
("grinding") can be found when the area is handled and manipulated.
Diagnosing these injuries is not usually difficult and radiographs are the best
way to determine the extent and type of fracture.
Treatment and Prognosis: In general, most significant fractures in the
tibia or femur of an adult horse are difficult to treat. Many of these horses
should be euthanized. This statement is also true for many fractures of the
femur in a foal. On the other hand, some minor fractures of the tibia can be
treated with only strict stall rest. The more complicated fractures of the tibia
and femur in a foal can sometimes be treated with surgery and/or cast
application. During the surgery, plates, screws, and pins may be used to hold
the fracture in place. There is no surgical treatment for fractures of the
pelvis. A fractured pelvis may be treated with strict stall rest for as long one
year. Slings may also be used for the first 6-8 weeks. Because there is such
variability in the types and treatments of these fractures, a veterinarian must
be involved in each individual case.
Again, no matter what type of fracture has
occurred, attention should be given to the opposite limb. In many cases, the
opposite limb will be forced to bear most of the weight. This can result in
laminitis and other problems.
Some foals with these types of fractures
do fairly well after successful treatment. If the horse is a yearling or adult,
the fracture has broken the skin, or the fracture is comminuted, the prognosis
is poor.
Problems in the Neck Region
- Wobbler Syndrome:
Introduction: The term "wobblers" is often used to describe
any condition of the horse where weakness and coordination problems are
involved. This condition can be caused by deformed vertebrae in the neck
(cervical vertebral malformations), equine protozoal myeloencephalitis
(EPM),
equine herpes, equine infectious anemia, trauma, and others. This discussion
will describe wobbler syndrome caused by deformed vertebrae in the neck. The
other conditions have been discussed elsewhere in this manual.
Causative Agent: Wobbler syndrome is caused by a defect in the
vertebrae of the neck that compresses the spinal cord. The deformed vertebrae
can compress the spinal cord all the time or only when the neck is flexed.
Studies indicate that this condition has some genetic and nutritional influences
that cause the vertebrae to not form properly. Horses that are fed high energy
diets, grow rapidly, and are large at a young age are more at risk.
Clinical Signs: Ataxia (balance problems), gait abnormalities, and
weakness are some of the common signs. Many horses are in pain and reluctant to
move their necks. Some horses recover and remain fairly normal, while others
digress to an unmanageable state.
Diagnosis: A physical exam will help to identify the possible location of
the problem. Radiographs are essential to determine exactly where the problems
are located and the severity of the deformities. These examinations may also
reveal degenerative joint disease (DJD) and osteochondritis dissecans (OCD)
lesions.
Treatment and Prognosis: Some mild cases may respond to anti-inflammatory
agents (steroids, bute) that help to reduce the inflammation in the spinal cord
and surrounding areas. This type of treatment only produces temporary
improvement, with the horse continuing to have problems. In most cases the
surgical treatment is a must. The surgical procedures that are commonly used are
designed to provide increased stability to the neck vertebrae. Most surgical
cases can return to breeding and a few horses may return to normal or near
normal function. Horses that show few clinical signs prior to surgery, have a
better chance of gaining a favorable recovery.
Problems Found in Many Different Joints and Locations
- Angular Limb Deformities:
Introduction: Angular deformities are defects where the limbs are
deviated in an abnormal position. These problems most often occur in young
animals. A section of the limb may be deviated away from the body (lateral
deviation or valgus deformity) or towards the body (medial deviation or varus
deformity). These deformities are most often found in the fetlock and carpus of
the front limbs. When an inward deviation of the limb above the knee and an
outward deviation of the limb below the knee takes place, it is called carpus
valgus or knock-kneed. A bowlegged animal is considered carpus varus.
Causative Agents: Congenital (present at birth) angular limb
deformities can be the result of nutritional imbalances of the mare, improper
positioning of the foal in the uterus, defective endochondral ossification, and
abnormal development of some of the bones associated with the joint. Acquired
angular limb deformities are developed during the first few months of life.
These can be caused by trauma or growth plate injuries, joint instability,
nutritional imbalances (too much or too little energy, phosphorus, and calcium),
defective endochondral ossification, abnormal development of some of the bones
associated with the joint, and abnormal weight bearing on a joint/growth plate
because of poor conformation, improper trimming, and excessive exercise.
To fully understand why these problems occur in growing animals, it is
necessary to have a basic knowledge of how long bones (radius, cannon, etc.) and
the small bones of the carpus (rows of carpal bones) are formed. Each long bone
in the body has a physis or growth plate. This is responsible for the up and
down (longitudinal) growth of each bone. Each long bone and the small cuboidal
bones of the carpus also rely on a process called endochondral ossification for
final bone maturation. Endochondral ossification is where cartilage (in the
epiphysis or ends of the long bones) actually ossifies to form bone. Any
process that injures the way the growth plate and endochondral ossification
function can result in angular limb deformities.
When abnormal amounts of
weight and pressure are placed on a growth plate or area of endochondral
ossification, the growth is stunted. For example, one way to cause a carpus
valgus deformity in a foal is to have an injury or poor conformation that causes
abnormal weight to be placed on the outside regions (lateral aspect) of the bone
(radius) above the knee (carpus) in the front limb. In this case, the outside
portion of the growth plate will NOT grow properly, while the inside (medial
aspect) will continue to grow. This causes the bone (radius) to cup or dish,
forcing the knees together. Nutritional imbalances, injury, and improper weight
bearing can also cause the growth plate to become inflamed (physitis) or even
close prematurely. This can result in abnormal growth and angular limb
deformities.
Clinical Signs: In severe cases, it is obvious that there is a problem
just by looking at the limbs. The horse may be lame and have swollen and painful
joints or growth plates.
Diagnosis: Radiographs are essential in identifying the location and
severity of the problem. A complete history should be taken and include the
following questions: Was the foal born this way? What is the diet? Was the mare
overweight during the pregnancy? Have there been any injuries to the limbs or
limb? A diagnosis can be reached based on the history, physical exam, and
radiographs.
Treatment: Treatment in all cases varies according to the cause of the
deformity. In general, there are three common avenues of treatment:
- Stall rest, corrective trimming, proper nutrition, and time. The
trimming should involve shortening the high side of the hoof wall. In carpus
valgus problems, this means shortening the outside (lateral) portion of the
hoof. Proper nutrition can include alfalfa hay, limited amounts of
concentrates, and access to a high phosphorus mineral supplement. For many of
the minor deformities, this may be all that is needed to correct the problem.
Many young foals will correct a deformity on their own within the first few
weeks of birth.
- Placing the affected limb in a tube or sleeve cast. This is commonly
used for joint instability problems.
- Surgical procedures. A surgical procedure called periosteal stripping is
commonly performed. During this procedure, the outer surface of the bone (periosteum)
is removed to stimulate bone growth. A different surgical procedure (sometimes
done on the same animal) called transphyseal bridging is also used. This is
where screw, wires, or staples are placed across one side of a growth plate to
prevent additional growth. These devices are removed once the deformity has
been corrected.
In general, if the problem is corrected early, most young foals have a
successful outcome.
Flexural Limb Deformities (Contracted Tendons):
Introduction: Flexural limb deformities are situations where the
various joints of the body are held in some degree of flexion. This is most
often the result of a contracted tendon. These problems are identified as
congenital (present at birth) or acquired (occurring after birth).
Causative Agents: Congenital deformities are most often caused
by malposition during the pregnancy, the mare ingesting toxic substances, and/or
inherited genetic defects. Acquired defects are often the result of pain
(epiphysitis, osteochondrosis, injury), genetics, nutritional imbalances
(excessive energy intake), and rapid growth. A combination of two or more of
these problems may also be the cause in some cases.
Clinical Signs and Diagnosis: In many cases more than one limb is
involved. Most of the time the knee (carpus) or fetlock is involved, and these
joints are often "popped" forward. The joint is held in this flexed
position, and may or may not be forced to a normal position with pressure. The
acquired cases will often result in a "club foot," where the horse
bears its weight on the toe.
Treatment for Congenital Deformities: Some horses will correct the
problem on their own with little or no human intervention. More complicated
cases can be helped/treated in one of three ways:
- By applying PVC splints to help "force" the joint back into
place. This should be done carefully, with plenty of padding and continual
observation. The PVC can be bent to accommodate the proper angles of the limb.
If care is not taken in the proper placement of these splints, sores and
injury can result.
- By applying a cast and potentially corrective shoes. This is reserved
for the more complicated cases and requires special attention by the owner and
veterinarian.
- Through surgical procedures. These surgical procedures are most often
used in the acquired flexural deformities and are not usually successful with
the congenital problems.
Treatment for Acquired Deformities: Some horses will correct the problem
on their own with exercise, proper nutrition, and corrective trimming. More
complicated cases are corrected through surgical procedures. The object behind
these procedures is to release tension placed on a contracted tendon. The common
procedures are flexor tenotomies and inferior check ligament desmotomies.
Arthritis, Osteoarthritis, and Osteochondritis:
Introduction: Arthritis is inflammation of a joint, which can be caused by
injury (trauma) or infection. If the arthritis is severe and untreated, it may
progress into degenerative joint disease (DJD) or osteoarthritis. Arthritis can
involve inflammation of the synovial membrane, joint capsule, cartilage, and
even bone. If both bone and cartilage are inflamed, it is called osteochondritis.
Causative Agents: A single or repeated injury to any joint in the body
can result in arthritis. This injury can be from excessive strain (racing,
working, etc.), or from a physical blow to the joint (kick, fall, etc.) causing
a fracture, sprain, or luxation. The most common causes of infectious arthritis
are bacteria (E-coli, Actinobacillus spp., Salmonella, Streptococcus spp.,
Pseudomonas spp, Corynebacterium equi, etc.) that invade the joint through a
wound or by the blood stream. These bacteria can enter the blood stream by an
umbilical infection, pneumonia, or other type of infection within the body.
Clinical Signs: In most cases, the affected joint will be hot, swollen,
and painful. The horse can be moderately to severely lame. When the problem
joint is flexed, the horse will often pull away, flinch, and act very painful.
Diagnosis: In both infectious and traumatic arthritis, it is important to
compare a normal joint with the problem joint. This can be done by palpating
(feeling) the normal and then the abnormal joint. Radiographs should also be
taken. To help with comparison, these radiographs should be taken of the normal
and abnormal joint in some circumstances. With the proper preparation and
technique, a veterinarian can take a sample of the joint fluid from a swollen
joint. This can be examined for evidence of infection (culture and sensitivity,
cell counts) and inflammation (increased protein, abnormal appearance). In some
cases an arthroscopic examination may need to be performed before a complete
diagnosis can made.
Treatment: For the traumatic causes of arthritis, the extent of the
damage must be identified with radiographs, and potentially, arthroscopy. Any
damaged cartilage, bone, or other joint structure must be removed or repaired.
The horse should be rested and some mild forms of flexion of the joint can be
used. Excessive hand walking should be avoided. Cold water hydrotherapy should
begin within 48 hours of the injury. This can involve cold water from a hose,
bathed over the affected joint for 15-20 minutes twice a day. After the initial
inflammation has gone down, the benefits of the cold water soaks are reduced.
Anti-inflammatory agents can also be used to help reduce the pain and
inflammation. Products like phenylbutazone (bute) and DMSO (Dimethyl sulfoxide)
are anti-inflammatory agents that can be administered by the owner. In some
cases injections of corticosteroids and Legend (hyaluronan) can be given
directly in the joint. Other joint protecting/healing products can also be
administered. These products include injectable polysulfated glycosaminoglycans
(Adequan) and oral glycosaminoglycans (Cosequin, Glyco-flex, and Power-Flex).
MSM is a naturally occurring sulfur compound that is a found in all living
things. It too can have a positive effect on the joints by reducing
inflammation. For additional information on many of these products, refer to
Section H of this manual.
In addition to many of the above
suggestions, arthritis that is due to an infection should be treated with
antibiotics.
Capped Hock, Capped Elbow (shoe-boil), Bicipital Bursitis
(shoulder), and Carpal Hygromas:
Introduction: These conditions are usually caused by injury to a bursa
resulting in bursitis. A bursa is a "cushion" between moving parts or
between various points of increased pressure (like between a bone and tendon).
When a bursa becomes irritated and inflamed it is called bursitis. Bursitis in
the hock is usually caused by the horse kicking something and hitting the point
of the hock. Bursitis in the elbow is often the result of a shoe coming up and
impacting the elbow. Hygromas in the knee (see figure 9) are also caused by
direct injury. In these cases, however, a bursa is not usually present before
the injury, but forms after repeated trauma.
| Figure 9: Carpal hygroma |
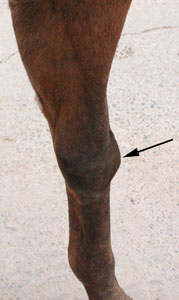 |
Clinical Signs: Some pain, heat, and swelling are the most common signs.
If the injury is significant, the swelling can be quite large and there can be
some soft tissue thickening.
Treatment: In most cases, the bursitis can be treated with ice packs,
anti-inflammatory agents, and rest. It is also important to prevent additional
injury to the bursa (remove the shoe on that foot, etc.). For more severe cases,
injections into the problem area and surgery may be required.
Epiphysitis:
Introduction: "Epiphysitis" is a problem that is commonly
found in young, growing animals (ages 4-8 months) and young horses beginning
training. The term "Epiphysitis" is somewhat misleading because the
problem actually involves the growth plate and not the end (epiphysis) of a long
bone.
Causative Agents: Fast growing, young animals that are fed high grain
rations seem to have the most problems. Genetics may also play a role in the
fact that faster growing foals experience epiphysitis. Abnormal weight bearing
and trauma/injury to the growth plate are sometimes associated with this
disease. Studies indicate that a combination of these influences is often the
cause. With the above being the known causes for epiphysitis, how they actually
cause the disease is less understood.
Clinical Signs: The most obvious sign is a "flaring" or
enlargement of the ends of the long bones. This commonly is seen above the knees
on the end of the radius. As the problem progresses, the end of the bone begins
to take on a "hour glass" shape. Depending on the severity of the
disease, the horse may or may not be lame. The horse may act painful when the
involved area is palpated or handled.
Diagnosis: Physical exam and radiographic images are often sufficient
to diagnose this problem.
Treatment and Prevention: The most important step in treating and
preventing this disease is to evaluate and adjust the horse’s ration. Any
nutritional imbalances should be corrected. Use the information found on page
A575 and the details contained below on nutrition to help calculate a proper
diet. Mineral analysis may need to be performed to determine any deficiencies or
excesses of the trace minerals. If the horse is over weight, restrict the amount
of energy being fed. Some horses may recover with rest and the proper use of
anti-inflammatory agents (bute). If anti-inflammatory agents are used, the foal will use the limb
more as the pain and inflammation is reduced.
This potentially can result in additional injury and epiphysitis. If radiographs show that
there are other problems (OCD lesions, angular limb deformities), these will
need to be corrected to help alleviate the epiphysitis. Many horses seem to
recover with time and rest; however, they never return to full performance
ability.
Luxations:
Introduction and Causative Agents: A luxation is a dislocation of a
joint and can occur in the fetlock, knee (carpus), shoulder, hock (tarsus),
stifle, and hip. These injuries most often occur when the limb is forced in an
abnormal direction. This can happen when the horse steps in a hole, falls,
slips, jumps, or twists the limb while in a flexed or extended position.
Clinical Signs: The limb that is involved often has a angular
deformity, where the portion of the limb distal to luxated joint is deviated
outward or inward. The joint itself maybe swollen, painful, and unstable. There
will also be varying degrees of lameness.
Diagnosis: Diagnosing the location of these injuries is not usually
difficult. Radiographs are the best way to confirm a diagnosis and determine if
any fractures are involved.
Treatment: Treatment for most luxations requires that the horse be
anesthetized and the dislocation be reduced or put back into place. This should
take place as soon as possible after the injury. Depending on the location of
the luxation, casts may also be applied. Any chip or other type of fracture
should be treated appropriately.
Prognosis: Many of the minor luxations where no fractures are involved
will often have a good recovery and return to performance. Luxations of the hip
joint, however, may never return to normal even after the head of the femur is
put back into place. If fractures, infection, or degenerative joint disease (DJD)
occur, the prognosis is poor.
Osteochondrosis, Osteochondritis Dissecans (OCD), and Subchondral Bone
Cysts:
Introduction: Osteochondrosis is a defect in the normal development of
cartilage. This defect occurs sometime in the process of endochondral
ossification. Endochondral ossification is where cartilage (in the epiphysis or
ends of the long bones) actually ossifies to form bone. If endochondral
ossification does not progress normally, defects called osteochondritis
dissecans (OCD) or subchondral bone cysts can result. OCD lesions are places
where fragments or flaps of cartilage associated with the joint are separated
from the rest of the cartilage. Bone cysts are areas in the end of the bone
where endochondral ossification does not progress normally. This leaves small
areas of cartilage deep within the end of the bone. These areas necrose or die
and leave a defect in the end of the bone.
Causative Agents: The following are thought to cause these defects in
a growing animal:
- Genetic influences.
- Nutritional imbalances (too much energy and mineral imbalances).
- Very rapid growth.
- Trauma and injuries.
It is sometimes difficult to identify just one specific cause for these
defects, so the problem may actually be a combination of the above.
Clinical Signs: OCD lesions are found in the following joints: the
stifle, hock (tarsus), shoulder, fetlock, knee (carpus), elbow, and hip. Bone
cysts are found in the following areas: the stifle, knee (carpus), hock
(tarsus), fetlock, pastern, coffin, shoulder, and elbow. In the case of OCD
lesions, the affected joint may be swollen, painful, and hot to the touch. The
horse is often lame. Cystic lesions are sometimes more difficult to diagnose.
These horses may or may not have swelling and lameness. If these signs do
appear, it is often after work, training, or exercise.
Diagnosis: Radiographs are essential in diagnosing these problems. In
many cases it is helpful to radiograph the opposite joint to use as a
comparison. Nuclear scintigraphy can also be used to help identify the problem
area.
Treatment: For some of the minor OCD and bone cyst problems, the horse
can be treated conservatively with rest and proper nutrition. Not all cases and
not all lesions will resolve by this approach. Some cases require that surgery (arthroscopic
or arthrotomy) be performed. For OCD lesions, the flap is removed and the area
of the defect cleaned.
Tedonitis ("bowed tendons"), Tenosynovitis, and Desmitis:
Introduction: Tendonitis is inflammation of a tendon, while desmitis is
inflammation of a ligament. The most common ligament problem is suspensory
ligament desmitis. Tenosynovitis is inflammation of the synovial lining of a
tendon sheath. In many instances, the inflammation includes not only the tendon
sheath but also the tendon itself.
Causative Agents and Clinical Signs: In most cases, these problems are
caused by severe straining and over-stretching of the tendon or ligament. This
can occur when excessive loads are placed on the limbs due to sudden turns,
jumping, stopping, or slipping. Things such as improper shoeing, poor
conformation, and traumatic injuries can also cause a problem to develop. When
injury occurs to the tendon, the tendon fibers can be damaged and the blood
supply can be compromised. Severe injury can result in complete rupture of the
tendon.
Clinical Signs: After the initial injury, the involved area is swollen,
painful, and hot to the touch. The horse is often lame and very painful when the
limb is flexed. These injuries can occur in the flexor tendons located behind
the cannon bone ("bowed tendon") in the area just below the knee or hock and
above the fetlock (see figure 10). In some cases it is an injury to the anular
ligament that causes the problem. The anular ligament wraps itself around the
fetlock area (kind of like shrink wrap) and helps to keep all the tendons and
joint structures encapsulated. If the anular ligament becomes inflamed, it may
begin to scar and shrink. The superficial flexor tendon runs just beneath this
anular ligament. If the anular ligament scars and constricts, the flexor tendon
is "pinched." This can be the cause of the swelling above a fetlock
joint. If these problems continue for prolonged periods of time, the tendon can
begin to scar and adhere to surrounding tissues. This will cause a loss of
function and flexibility of the tendon/ligament. In some cases the navicular and
sesamoid bones may be involved. If the sesamoids are inflamed, it is called
sesamoiditis.
| Figure 10: Bowed tendon |
 |
Diagnosis: Many cases are identified based on physical exam and
clinical signs. The severity of the problem can often be determined through the
use of ultrasound and radiography.
Treatment: The key to healing acute tendon/ligament problems is to reduce
the inflammation and keep any additional trauma and swelling from occurring.
Treatments to reduce the inflammation include cold water soaks or ice packs for
20 minutes twice a day for the first 2-3 days and anti-inflammatory agents (bute).
Topical DMSO can also be beneficial in reducing the swelling. Pressure wraps and
even casting can be used in more severe cases to prevent additional stretching
and injury to any of the tendons and ligaments. To prevent additional injury,
strict stall rest (for the first two weeks), followed by mild manipulations of
the injured area, should be used. To help build the tendon, regularly pick up the
foot/leg and move it gently through a series of flexing motions.
Excessive flexion, particularly where the horse shows pain, will cause continued
damage and should be avoided.
After the rest and mild manipulations, carefully choose what activities the
horse is asked to perform. These should be low impact and preferably without a
rider. Some minor tendon stretching will occur with normal use. After
these occasions, reduce the chance for inflammation and swelling by using cold
water soaks and anti-inflammatory agents as needed. If continued irritation
occurs, scaring and permanent injury will result.
For the more chronic tendon/ligament injuries, where scarring and boney damage
may be involved, surgical intervention is often required. There are many
different procedures that can be used. An equine surgeon will need to evaluate
each situation before a recommendation can be given. The usual treatment for
bowed tendons caused by anular ligament problems is a surgical procedure where
the anular ligament is cut. This allows the flexor tendons to move more freely.
Nutrition and Supplements:
Proper nutrition plays an essential role in the development of healthy bones,
muscles, and related structures. Consuming rations that contain imbalances in
protein, minerals, and vitamins can cause abnormal bone development. Too much
feed intake can be as detrimental as too little feed intake. Because most of the
nutrition related problems occur in foals, attention should be given to the
ration being fed to a pregnant/lactating mare. In general, if the mare does not
consume sufficient amounts of a properly balanced diet, overall milk production
will be low, and the milk will lack the essential vitamins and minerals
(calcium, phosphorus, vitamin A, copper) necessary for a healthy foal. If the
mare consumes too much high quality feed, she will be overweight and still not
produce sufficient quantities of milk for the foal because of excess fat
deposits in the mammary gland. An overweight mare will also not breed back as
well.
Pregnant mares and ones that are lactating should be feed a diet that is at
least 12-14% protein on a dry matter basis. Their milk should contain 80-120
mg/dl of calcium and 45-90 mg/dl of phosphorus. They should be fed a balanced
ration that contains vitamin A, copper, zinc, and possibly manganese. Because
the mare’s ability to produce sufficient quantities of milk declines with
time, it is important to begin creep feeding foals at a young age (3-4 weeks).
Remember, however, that feeding foals excess protein (greater than 2% of the
foals requirement), zinc, selenium, and iodized salt, can result in bone, hoof,
and hair problems. Additional information on creep feeding and nutrition can be
found on pages A249 and A575.
In many cases, the use of dietary supplements is not necessary and can even
be detrimental to the horse. This statement is true only if the horse has access
to sufficient amounts of a balanced diet. Supplements should be used when a
deficiency in the diet is present, a specific joint disease is diagnosed, or
when the horse has the potential to develop a joint, muscle, or tendon problem.
To fully understand the common supplements that are used to maintain healthy
joints, it is important to know something about what makes a healthy joint. Many
of the joints in the body (knee, hock, fetlock, etc.) contain cartilage and
synovial or joint fluid. These joints are surrounded by a synovial membrane and joint
capsule. Healthy cartilage and synovial fluid are essential in order to provide
a low friction, smooth surface for the bones of the joint to move against and
impact with. Realize that stresses placed on the joint during training and
competition cause wear and tear to the joint cartilage and inflammation. If
damage is severe or the inflammation continues for extended periods of time, the
cartilage and joint can be permanently injured.
Articular cartilage has the ability to replenish itself when mild damage
occurs. It does this by producing collagen and proteoglycans. Collagen is a
protein that provides the strength of cartilage, while proteoglycans (made of
glycosaminoglycans) provide resistance to compressive forces. Most of the joint
supplements contain raw materials or nutrients that are required to allow the
cartilage to replenish itself and ingredients that help reduce inflammation in
the joint. Glucosamine HCI, chondroitin sulfate, and methylsulfonylmethane (MSM)
are some of these ingredients. Glucosamine is required for the production of
glycosaminoglycans and proteoglycans. It also helps reduce
inflammation. Chondroitin sulfate is one of the major glycosaminoglycans found
in cartilage and also helps to reduce inflammation. Methylsulfonylmethane (MSM)
acts as an anti-inflammatory and general pain reliever.
The following list identifies some common joint/muscle/tendon supplements
that can be useful in many horses:
- Methylsulfonylmethane (MSM) - See page H506 for additional details.
- Cosequin - See page H126 for additional details.
- Glyco-Flex - See page H280 for more information.
- Power-Flex - See page H645 for more information.
The following are products that can be injected or given orally to help
relieve joint inflammation and pain:
- Adequan (Polysulfated glycosaminoglycan) - See page H10.
- Hyaluronic acid (Legend) - This product is given as an injection. It is
important for healthy synovial fluid and acts as an anti-inflammatory agent.
- Phenylbutazone (bute) - See page G90 for more information.
- Corticosteroids (triamcinolone - Vetalog; betamethasone - Betvet;
methylprednisolone - Depo-Medrol) - All of these act as anti-inflammatory
agents and should be administered by a veterinarian.
Summary: In conclusion, joint, bone, tendon, and ligament injuries can
often be challenging problems to diagnose and resolve. If a problem does not
improve with routine treatments, be sure to involve a local veterinarian.












